How Would You Treat Bursitis In Ball Of Foot
A Bursa is a small fluid filled sac that forms in areas of extra rubbing and friction. They are usually present with a bone deformity as the bone is pressed against other structures like a tendon or against the ground as you walk. The bursa acts as a shock absorber and is a way for your body to protect you from damage. When this bursa or sac like structure becomes swollen and inflammed it is called bursitis. The bursa may be anatomical meaning normally present, or it may be adventitious meaning, only present because of a problem. Many bursa are present and do not cause pain.
Causes
Occasionally the bursal sac can become inflamed and painful. Pain to the region is worse typically with initial weight bearing activity such as rising from bed in the morning. Swelling and warmth to the region are common. Clinical examination shows pain to palpation at the retrocalcaneus at a level just before the Achilles tendon. Increase pressure and friction of the Achilles tendon across the retrocalcaneal region is the cause of this bursitis. A high arch, tight Achilles tendon or bone spur appear to be some of the main causes of this problem. With a high arch the back portion of the calcaneus abnormally projects into the Achilles tendon region.
Symptoms
Limping. Decreased movement. Your ankles may feel stiff or unable to move as well as they usually do. Pain or tenderness in the back of the ankle. It may be worse at the beginning of exercise, or when running uphill. You may also have pain when wearing shoes. Redness and warmth. If the bursa is infected, the skin over the heel may be red and warm. You may also have a fever. Swelling on the back of the heel.
Diagnosis
Bursitis is usually diagnosed after a careful physical examination and a full review of your medical history. If you garden and spend a lot of time on your knees, or if you have rheumatoid arthritis, tell your doctor, this information can be very helpful. During the physical exam, he or she will press on different spots around the joint that hurts. The goal is to locate the specific bursa that is causing the problem. The doctor will also test your range of motion in the affected joint. Other tests usually aren?t required to diagnose bursitis, but your doctor may suggest an MRI, X-ray or ultrasound to rule out other potential causes of pain.
Non Surgical Treatment
The patient with retrocalcaneal bursitis should be instructed to apply ice to the posterior heel and ankle in the acute period of the bursitis. Icing can be performed several times a day, for 15-20 minutes each. Some clinicians also advocate the use of contrast baths. Gradual progressive stretching of the Achilles tendon may help relieve impingement on the subtendinous bursa and can be performed in the following manner. Stand in front of a wall, with the affected foot flat on the floor. Lean forward toward the wall until a gentle stretching is felt within the ipsilateral Achilles tendon. Maintain the stretch for 20-60 seconds and then relax. Perform the stretches with the knee extended and then again with the knee flexed. To maximize the benefit of the stretching program, repeat the above steps for several stretches per set, several times daily. Avoid ballistic (ie, abrupt, jerking) stretches. Other treatment options are microcurrent therapy and corticosteriod injection into the retrocalcaneal bursa. If conservation treatment fails then surgery is indicated.
Surgical Treatment
Surgery. Though rare, particularly challenging cases of retrocalcaneal bursitis might warrant a bursectomy, in which the troublesome bursa is removed from the back of the ankle. Surgery can be effective, but operating on this boney area can cause complications, such as trouble with skin healing at the incision site. In addition to removing the bursa, a doctor may use the surgery to treat another condition associated with the retrocalcaneal bursitis. For example, a surgeon may remove a sliver of bone from the back of the heel to alter foot mechanics and reduce future friction. Any bone spurs located where the Achilles attaches to the heel may also be removed. Regardless of the conservative treatment that is provided, it is important to wait until all pain and swelling around the back of the heel is gone before resuming activities. This may take several weeks. Once symptoms are gone, a patient may make a gradual return to his or her activity level before their bursitis symptoms began. Returning to activities that cause friction or stress on the bursa before it is healed will likely cause bursitis symptoms to flare up again.
Help For Contracted Toes Feet
 Overview
Overview
A Hammer toes is a contracture-or bending-of the toe at the first joint of the digit, called the proximal interphalangeal joint. This bending causes the toe to appear like an upside-down V when looked at from the side. Any toe can be involved, but the condition usually affects the second through fifth toes, known as the lesser digits. Hammertoes are more common to females than males.
Causes
The APMA says that hammertoe can result from a muscle imbalance in the foot that puts undue pressure on the joints, ultimately causing deformity. Inherited factors can contribute to the likelihood of developing hammertoe. Arthritis, stroke or nerve damage from diabetes or toe injuries such as jamming or breaking a toe can affect muscle balance in the foot, leading to hammertoe. The Mayo Clinic says that wearing improper shoes often causes hammertoe. Shoes that squeeze the toes, such as those with a tight toe box or with heels higher than two inches, can put too much pressure on the toe joints.
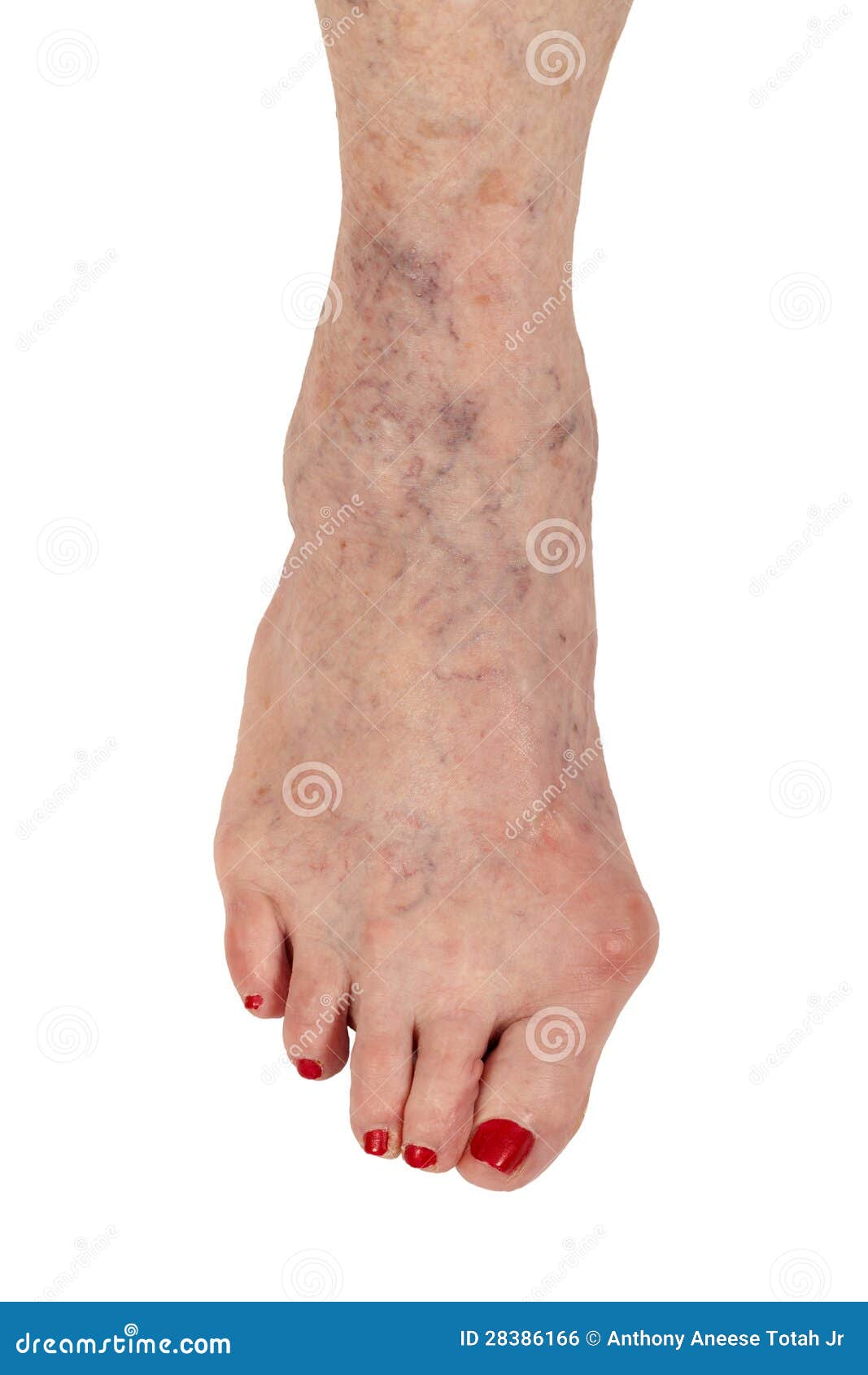 Symptoms
Symptoms
Symptoms of a hammertoe are usually first noticed as a corn on the top of the toe or at the tip which produces pain with walking or wearing tight shoes. Most people feel a corn is due to a skin problem on their toes, which in fact, it is protecting the underlying bone deformity. A corn on the toe is sometimes referred to as a heloma dura or heloma durum, meaning hard corn. This is most common at the level of the hammertoes affected joint due to continuous friction of the deformity against your shoes.
Diagnosis
The treatment options vary with the type and severity of each hammer toe, although identifying the deformity early in its development is important to avoid surgery. Your podiatric physician will examine and X-ray the affected area and recommend a treatment plan specific to your condition.
Non Surgical Treatment
A toe doctor can provide you with devices such as hammer toe regulators or straighteners. These are also available for purchase locally. Another good idea is to start the hammer toe rehabilitation process by gently trying to straighten the joint and moving and flexing the affected toe as much as possible without straining it. If hammer toe taping doesn?t work, you may require surgery. If the joints and tendons have stiffened to a point of non-movement, hammer toe corrective surgery may need to enter the toe and either cut or manually move some of the tendons and ligaments. Although the treatment is relatively safe fast, you may deal with some stiffness afterwards.
Surgical Treatment
Curative treatment of hammertoes varies depending upon the severity of the deformity. When the hammertoe is flexible, a simple tendon release in the toe works well. The recovery is rapid often requiring nothing more that a single stitch and a Band-Aid. Of course if several toes are done at the same time, the recovery make take a bit longer.
 Prevention
Prevention
Hammertoe can usually be prevented by wearing shoes that fit properly and give the toes plenty of room. Don?t wear shoes with pointed or narrow toes. Don?t wear shoes that are too tight or short. Don?t wear high-heeled shoes, which can force the toes forward. Choose shoes with wide or boxy toes. Choose shoes that are a half-inch longer than your longest toe. If shoes hurt, don?t wear them.
The Treatment And Cause Of Over-Pronation Of The Feet
Pronation is the inward movement of the foot as it rolls to distribute the force of impact of the ground as you run. The foot "rolls" inward about fifteen percent, comes in complete contact with the ground, and can support your body weight without any problem. Pronation is critical to proper shock absorption, and it helps you push off evenly from the front of the foot. Although pronation is a natural movement of the foot, the size of the arch can affect its ability to roll, causing either supination (underpronation) or overpronation. If you have a normal arch, you're likely a normal pronator, meaning you'll do best in a shoe that offers moderate pronation control. People with flat feet normally overpronate, so they do well in a motion-control shoe that controls pronation. High-arched people typically underpronate, so they do best in a neutral-cushioned shoe that encourages a more natural foot motion.

Causes
Over-pronation has different causes. Obesity, pregnancy, age or repetitive pounding on a hard surface can weaken the arch leading to over-pronation. Over-pronation is also very common with athletes, especially runners and most of them nowadays use orthotics inside their shoes. Over-pronation affects millions of people and contributes to a range of common complaints including sore, aching feet, ball of foot pain, heel Pain, achilles tendonitis, bunions, shin pain, tired, aching legs, knee pain and lower back pain. The most effective treatment solution for over-pronation is wearing an orthotic shoe insert. Orthotics correct over-pronation, thereby providing natural, lasting pain relief from many common biomechanical complaints.
Symptoms
In addition to problems overpronation causes in the feet, it can also create issues in the calf muscles and lower legs. The calf muscles, which attach to the heel via the Achilles tendon, can become twisted and irritated as a result of the heel rolling excessively toward the midline of the body. Over time this can lead to inflexibility of the calf muscles and the Achilles tendon, which will likely lead to another common problem in the foot and ankle complex, the inability to dorsiflex. As such, overpronation is intrinsically linked to the inability to dorsiflex.
Diagnosis
If you cannot afford to get a proper gait analysis completed, having someone observe you on a treadmill from behind will give you an idea if you are an overpronator. It is possible to tell without observing directly whether you are likely to be an overpronator by looking at your foot arches. Check your foot arch height by standing in water and then on a wet floor or piece of paper which will show your footprint. If your footprints show little to no narrowing in the middle, then you have flat feet or fallen arches. This makes it highly likely that you will overpronate to some degree when running. If you have low or fallen arches, you should get your gait checked to see how much you overpronate, and whether you need to take steps to reduce the level to which you overpronate. Another good test is to have a look at the wear pattern on an old pair of trainers. Overpronators will wear out the outside of the heel and the inside of the toe more quickly than other parts of the shoe. If the wear is quite even, you are likely to have a neutral running gait. Wear primarily down the outside edge means that you are a supinator. When you replace your running shoes you may benefit from shoes for overpronation. Motion control or stability running shoes are usually the best bet to deal with overpronation.

Non Surgical Treatment
There are exercises that you can do to help deal with the effects and treat the cause. Obviously you can opt for an insert into your shoe either by way of your sports shop or go see a podiatrist. Like anything in your body that is not working correctly; you will have to manage your condition. Don't put off dealing with the problem as it will manifest associated issues along the alignment and as far up as your neck. If it's mild pronantion, I suggest running barefoot. If you can't do this then don't wear shoes at all at home or in the office as much as possible. Give your calf muscles a huge stretch everyday as these with the ligaments from the foot up to the muscle get tight and are linked to your pain. Loosen your calf muscles as much as possible. Great exercise is to sit barefoot with a marble on the floor in front of you. Grab the marble with your toes and try to hold it tight in the middle of the base of your foot. Ping pong balls and even golf balls work. Do this each night and combined with calf stretches you'll start to correct the muscle alignment gradually in the foot. Put more attention into massaging your feet, standing with a good posture, stretching your feet, ankles and calf muscles. Lastly, if you are fat this will not help at all. You must lose weight swimming, cycling and eradicating sugar and fat from your diet. The added strain on the foot by being a fat body compounds the problems and inhibits corrective results that you are after.
Surgical Treatment
Depending on the severity of your condition, your surgeon may recommend one or more treatment options. Ultimately, however, it's YOUR decision as to which makes the most sense to you. There are many resources available online and elsewhere for you to research the various options and make an informed decision.
Physical Therapy For Severs Disease
Sever's disease, also known as calcaneal apophysitis, is a medical condition that causes heel pain in one or both feet of children during the period when their feet are growing. Sever's disease occurs most commonly in boys and girls between the ages of 8 and 14 years of age. Sever's disease occurs when the part of the child's heel known as the growth plate, or the calcaneal epiphysis, an area attached to the Achilles tendon, suffers an injury or when the muscles and tendons of the growing foot do not keep pace with bone growth. The result is constant pain experienced at the back of the heel and the inability to put any weight on the heel, forcing the child to bear weight on their toes while walking. A toe gait develops in which the child must change the way they walk to avoid placing weight on the painful heel, a position that can lead to other developmental problems.
Causes
Children are at greatest risk of developing Sever's disease when they have reached the early part of a growth spurt in early puberty. For girls, this is typically around ages 8 to 10. For boys, it happens somewhere between the ages of 10 to 12. By the age of 15, the back of the heel has typically stopped growing in most children, and Sever's disease becomes rare. Any running or jumping activities can increase the odds that a child will develop Sever's disease. Soccer and gymnastics are two common sports that tend to put kids at risk.
Symptoms
Pain is usually related to activity levels. In most cases the posterior aspect of the calcaneus will be tender. Checking both the medial and lateral aspects of the posterior portion of the growth plate will often show tenderness. Occasionally, the plantar aspect may be tender or both of these locations may be found to be tender. Frequently the Achilles tendon is tight and there may have been a recent increase in activity. The factors contributing to this disorder are similar to those causing plantar fasciitis, but a tight Achilles tendon appears to be a greater contributor than pronation.
Diagnosis
A doctor or other health professional such as a physiotherapist can diagnose Sever?s disease by asking the young person to describe their symptoms and by conducting a physical examination. In some instances, an x-ray may be necessary to rule out other causes of heel pain, such as heel fractures. Sever?s disease does not show on an x-ray because the damage is in the cartilage.
Non Surgical Treatment
Primary treatment involves the use of heel cups or orthotics with a sturdy, supportive plastic shell. Treatment may also include cutting back on sports activities if pain interferes with performance, calf muscle stretching exercises, icing, and occasionally anti-inflammatory medications. Severe cases may require the short term use of a walking boot or cast.
Exercise
Exercises that help to stretch the calf muscles and hamstrings are effective at treating Sever's disease. An exercise known as foot curling, in which the foot is pointed away from the body, then curled toward the body in order to help stretch the muscles, has also proven to be very effective at treating Sever's disease. The curling exercise should be done in sets of 10 or 20 repetitions, and repeated several times throughout the day.
What Will Be The Signs Or Symptoms Of A Ruptured Achilles Tendon?
Overview
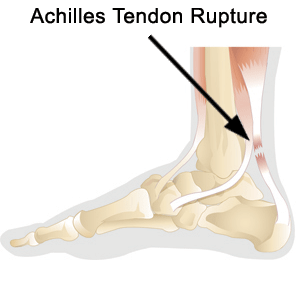 The Achilles tendon is the largest and most vulnerable tendon in the body. It joins the gastrocnemius (calf) and the soleus muscles of the lower leg to heel of the foot. The gastrocnemius muscle crosses the knee, the ankle, and the subtalar joints and can create stress and tension in the Achilles tendon . Tendons are strong, but not very flexible so they can only so far before they get inflammed and tear or rupture.
The Achilles tendon is the largest and most vulnerable tendon in the body. It joins the gastrocnemius (calf) and the soleus muscles of the lower leg to heel of the foot. The gastrocnemius muscle crosses the knee, the ankle, and the subtalar joints and can create stress and tension in the Achilles tendon . Tendons are strong, but not very flexible so they can only so far before they get inflammed and tear or rupture.
Causes
The Achilles tendon is most commonly injured by sudden plantarflexion or dorsiflexion of the ankle, or by forced dorsiflexion of the ankle outside its normal range of motion. Other mechanisms by which the Achilles can be torn involve sudden direct trauma to the tendon, or sudden activation of the Achilles after atrophy from prolonged periods of inactivity. Some other common tears can occur from overuse while participating in intense sports. Twisting or jerking motions can also contribute to injury. Fluoroquinolone antibiotics, famously ciprofloxacin, are known to increase the risk of tendon rupture, particularly achilles.
Symptoms
Tendon strain or tendon inflammation (tendonitis) can occur from tendon injury or overuse and can lead to a rupture. Call your doctor if you have signs of minor tendon problems. Minor tenderness and possible swelling increases with activity. There is usually no specific event causing sudden pain and no obvious gap in the tendon. You can still walk or stand on your toes. Acute calf pain and swelling can indicate a tear or partial tear of the Achilles tendon where it meets the calf muscle. You may still be able to use that foot to walk, but you will need to see a specialist such as an orthopedic surgeon. Surgery is not usually done for partial tears. Sometimes special heel pads or orthotics in your shoes may help. Follow up with your doctor to check for tendonitis or strain before resuming activity, because both can increase the risk of tendon rupture. Any acute injury causing pain, swelling, and difficulty with weight-bearing activities such as standing and walking may indicate you have a tear in your Achilles tendon. Seek prompt medical attention from your doctor or emergency department. Do not delay! Early treatment results in better outcome. If you have any question or uncertainty, get it checked.
Diagnosis
During the clinical examination, the patient will have significantly reduced ankle plantar flexion strength on the involved side. When the tendon is palpated with one finger on either side, the tendon can be followed from the calcaneus to where it "disappears" in the area of the rupture and to where it then returns 2 to 3 cm proximal to the rupture. If the injury is recent, the patient indicates that her pain is localized at the site of the rupture. The defect eventually fills with blood and edema and the skin over the area becomes ecchymotic.
Non Surgical Treatment
The most widely used method of non-surgical treatment involves the use of serial casting with gradual progression from plantar flexion to neutral or using a solid removable boot with heel inserts to bring the ends of the tendon closer together. The advantage of a solid removable boot is that it allows the patient to begin early motion and is removable. Wide variability exists among surgeons in regards to the period of absolute immobilization, initiating range of motion exercises, and progression of weight bearing status. 
Surgical Treatment
While it is possible to treat an Achilles tendon rupture without surgery, this is not ideal since the maximum strength of the muscle and tendon rarely returns. The reason is the ends of the tendon are ruptured in a very irregular manner, almost like the ends of a paint brush. As soon as the tendon ruptures, the calf muscle (gastrocnemius muscle) continues to pull on the tendon and the end of the ruptured tendon pulls back into the leg, which is called retraction. Once the tendon retracts, it is never possible to get sufficient strength back without surgery, because the muscle no longer functions at the correct biomechanical length and is now stretched out. There are patients for whom surgery cannot be performed, in particular, due to existing medical conditions that may add to potential for complications following surgery. For these patients, a specially designed boot that positions the foot correctly and takes the pressure and tension off the muscle and tendon is used. Most importantly, a cast is never used because it causes permanent shrinkage (atrophy) of the calf muscle. The special boot permits pressure on the foot with walking. The boot also has a hinge to permit movement of the ankle. Many studies of Achilles tendon ruptures have shown that this movement of the foot in the boot while walking is ideal for tendon healing. If surgery is not recommended, it is essential to obtain special tests to check that the ends of the tendon are lying next to each other so that healing can occur. The best test to do this is an ultrasound and not an MRI.
Prevention
Achilles tendon rupture can be prevented by avoiding chronic injury to the Achilles tendon (i.e. tendonitis), as well as being careful to warm up and stretch properly before physical activity. Additionally, be sure to use properly fitting equipment (e.g. running shoes) and correct training techniques to avoid this problem!